Who We Are
Legal Services of Northern Michigan
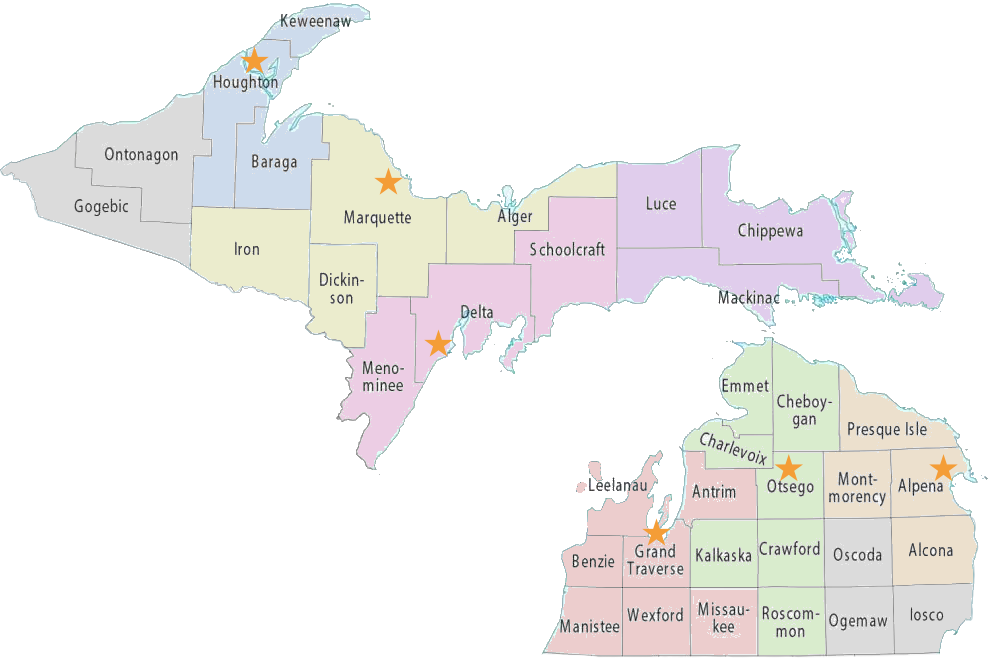
Established in 1966, Legal Services of Northern Michigan fills gaps in the civil justice system that prevent low income and marginalized communities from accessing legal representation. We have a staff of 15 experienced and dedicated lawyers, plus support staff, located at 6 offices throughout 36 counties in Northern Lower Michigan and the Upper Peninsula.
Our clients include people:
- facing evictions and foreclosures
- seeking safety from domestic violence, sexual assault, and elder abuse
- trying to access benefits that deliver basic income, healthcare, and food security
- many others facing civil legal problems that threaten basic needs or personal safety
LSNM is guided by a Board of Directors consisting of attorneys, former clients, and representatives of partner agencies. Quarterly meetings are held usually in March, June, September, and December. Contact any office for information about the next board meeting.
LSNM is managed by Kenneth Penokie, Executive Director, with the assistance of two Deputy Directors, Mary Kavanaugh-Gahn and Kirsten L. Keilitz.